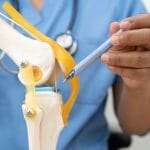
By Mr. Javier Waterman, Registered Physiotherapist
Joint mobilisation is a fundamental manual therapy technique used by physical therapists to restore normal movement, reduce pain, and improve overall joint function. Whether following an injury, surgery, or due to chronic conditions like arthritis, restricted joint mobility can significantly affect a person’s ability to perform daily activities and maintain a good quality of life. Through skilled, controlled movement of the joints, mobilisation helps to re-establish normal motion, reduce stiffness, and ease discomfort, allowing you to move with more freedom and confidence.
Understanding Joint Mobilisation
Joint mobilisation involves the application of passive, rhythmic movements to a joint within its natural range of motion. Unlike manipulation which is a single, quick thrust beyond the joint’s normal limit, joint mobilisation uses slower, graded movements that target specific restrictions in the joint capsule, surrounding ligaments, and soft tissues.
The technique is grounded in the principles of biomechanics and neurophysiology. When a joint becomes stiff or restricted the surrounding tissues adapt to this limitation and pain often develops due to increased strain, inflammation, or poor movement patterns. Mobilisation addresses these mechanical and neurological components, promoting smoother joint mechanics and reducing pain transmitted to the central nervous system.
How It Works
The process of joint mobilisation is based on applying small oscillatory movements or sustained stretches at varying intensities, commonly categorized into grades 1 through 3
● Grades 1 (loosening)- Short amplitude oscillatory movements performed within the joint’s available range to help relieve pain
● Grades 2 (tightening) Used where joint range is limited by pain and muscle spasm rather than shortened tissues
● Grade 3 (stretching) are larger amplitude or sustained movements aimed at stretching tight tissues and increasing range of motion.
These movements stimulate the joint’s mechanoreceptors which are specialized nerve endings that detect motion and pressure. Activation of these receptors can help reduce pain perception through a process called pain gate control, in which non-painful input closes the nerve “gates” to painful input, effectively diminishing the sensation of pain. Additionally, mobilisation improves the flow of synovial fluid, which nourishes cartilage and reduces friction, further supporting pain relief and movement restoration.
Benefits of Joint Mobilisation
1. Increased Range of Motion By addressing capsular tightness and soft tissue restrictions, mobilisation helps restore the joint’s normal movement. This is particularly beneficial in conditions like post-surgical stiffness, frozen shoulder, or after periods of immobilization.
2. Pain Reduction Mobilisation reduces pain both mechanically and neurologically, by desensitizing pain receptors and promoting endorphin release.
3. Improved Function and Mobility With reduced pain and improved motion you can perform everyday activities more efficiently, enhancing overall function and independence.
4. Enhanced Circulation and Joint Nutrition Gentle movement increases local blood flow and synovial fluid exchange, aiding tissue healing and maintaining cartilage health.
5. Reduced Muscle Tension Mobilisation can help relax muscles around the joint, reducing protective spasms and encouraging more balanced movement patterns.
Clinical Applications
Joint mobilisation can be used across a wide range of conditions, including:
● Osteoarthritis and degenerative joint disease – to ease stiffness and maintain joint mobility.
● Post-injury or post-surgical stiffness – such as following fractures, sprains, or joint replacements.
● Neck and back pain – to alleviate restricted vertebral motion and associated muscle tension.
● Shoulder, knee, and ankle dysfunctions – to restore normal biomechanics after injury or overuse.
● Neurological rehabilitation – in cases where joint mobility aids balance, posture, and gait retraining.
Each treatment plan is tailored to the your specific needs, taking into account the cause of restriction, stage of healing, pain levels, and overall health. Mobilisation is often integrated with other therapeutic techniques such as stretching, strengthening, and patient education for optimal outcomes.
Safety and Professional Application
Joint mobilisation should always be performed by a trained physical therapist or manual therapy professional. Improper technique or excessive force can cause discomfort or exacerbate the condition. Therapists assess each joint carefully, testing for stability, pain response, and range before applying mobilisations. Contraindications include acute inflammation, fractures, hypermobility, or certain systemic diseases that affect bone or joint integrity.
Communication between therapist and patient is essential throughout the process. The patient should feel a gentle stretch or movement, but not sharp or severe pain. When properly applied, mobilisation is a safe and effective component of a comprehensive rehabilitation program.
Conclusion
Joint mobilisation remains important for the physiotherapy practice for its effectiveness in restoring motion, easing pain, and enhancing quality of life. By addressing both the mechanical restrictions of the joint and the neurological factors influencing pain, this technique promotes natural healing and functional recovery.
For individuals struggling with stiffness, chronic pain, or movement limitations, working with a qualified physical therapist to incorporate joint mobilisation into their care plan can be a powerful step toward better mobility and lasting relief.

Leave a Comment